An update on Medical Yarn Ups in the Northern Territory
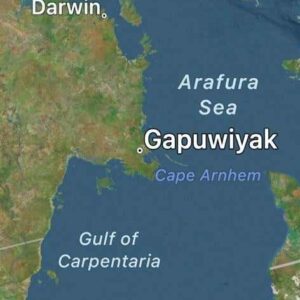
A postcard from Gapuwiyak, Arnhem Land, Northern Territory - Yolnu Country
Professor Bob Morgan, a proud, senior Gamilaroi man and I travelled over 500 kilometres east of Darwin to the Arnhem Land community of Gapuwiyak to continue our work helping in the Northern Territory with Medical Yarn Ups (MYUs).
We were in the company of Dr Lou Sanderson, the Medical Director of Miwatj Aboriginal Health Corporation and Kellie Kerin from Aboriginal Medical Services Alliance Northern Territory (AMSANT), both with vast passion and experience working in Northern Territory remote communities.
We had been invited by Miwatj Aboriginal Health Corporation and the small Yolnu community of roughly 800 to yarn about MYUs.
MYUs (a form of Shared Medical Appointment) are not only a process to delivery medical consultations but are also an enduring, Aboriginal and Torres Strait Islander model of care that brings together groups of people with similar concerns, managed by a trusted facilitator, with their healer, in this case the GP. In addition, others in the group are listening, sharing and encouraged to contribute their knowledge and experiences.
We were treated to a most moving and generous Welcome to Country and smoking ceremony. We were also introduced to the Tradition Owners of Gapuwiyak. They gave us permission and their blessings to conduct our work and thus began three days of yarning with the community and clinical staff about MYUs.
There was a palpable excitement about this approach to healthcare among everyone we spoke to, especially the Aboriginal staff.
MYUs make it possible to practice more Lifestyle Medicine and potentially prevent and better manage lifestyle-related illness such as Type 2 Diabetes Mellitus and renal disease, both of which are over-represented in Gapuwiyak and most other First Nations communities. The rate of Type 2 Diabetes Mellitus being up to five times the rate of Non-Aboriginal Australians. In one community we have visited previously in the Nothern Territory, the rate was 80%, with 50% of the community suffering kidney disease as well.
In one shocking statistic, remote living Aboriginal women are 29 times more likely to die from kidney disease than Non-Aboriginal women.
Lifestyle Medicine is the best medicine we have.
Medical Yarn Ups provide the opportunity to deliver the care that is needed for preventing and managing lifestyle-related illness.
And, importantly, MYUs are a First Nation’s model of care that has the potential to change current colonised-derived models and ways of doing health ‘on’ First Nation’s people so that Aboriginal and Torres Strait Islander people and communities have greater opportunity to take the lead in managing their health.
In this way Non-Indigenous allies and the Health Services can do more health work ‘with’ Aboriginal and Torres Strait Islander people. This is a desire we heard many times in our conversations with the clinic staff and the community.
Lifestyle Medicine and MYUs provide a vehicle that can have Aboriginal and Torres Strait Islander people drive self-determination and health improvement, and that will eventually be how the Gap closes.
Let’s close the Gap in Gapuwiyak and everywhere else in Australia.

John Stevens
John Stevens RN, PhD, FACN, FASLM, currently leads the discipline of Lifestyle Medicine at Southern Cross University. He is a Medical Sociologist, a 40-year Registered Nurse and works as a consultant to industry on the implementation of models of care that improve the prevention, management and reversal of lifestyle-related chronic illness by supporting healthcare workers to integrate lifestyle medicine into practice. John is a founder and director of the Australasian Society of Lifestyle Medicine (ASLM), which he and his colleagues officially established in 2008. John has been pioneering Shared Medical Appointments (aka Group Consultations and Medical Yarn Ups) in Australia and New Zealand and has been acknowledged by his peers with a Lifestyle Medicine, Outstanding Achievement Award for his contribution to the well-being of the community through this work. John has over 100 published articles in matters relating to Lifestyle Medicine and is regularly invited to speak at conferences and public events. He lives and thrives in the rural town of Mullumbimby, NSW, Australia, with his wife and five children.